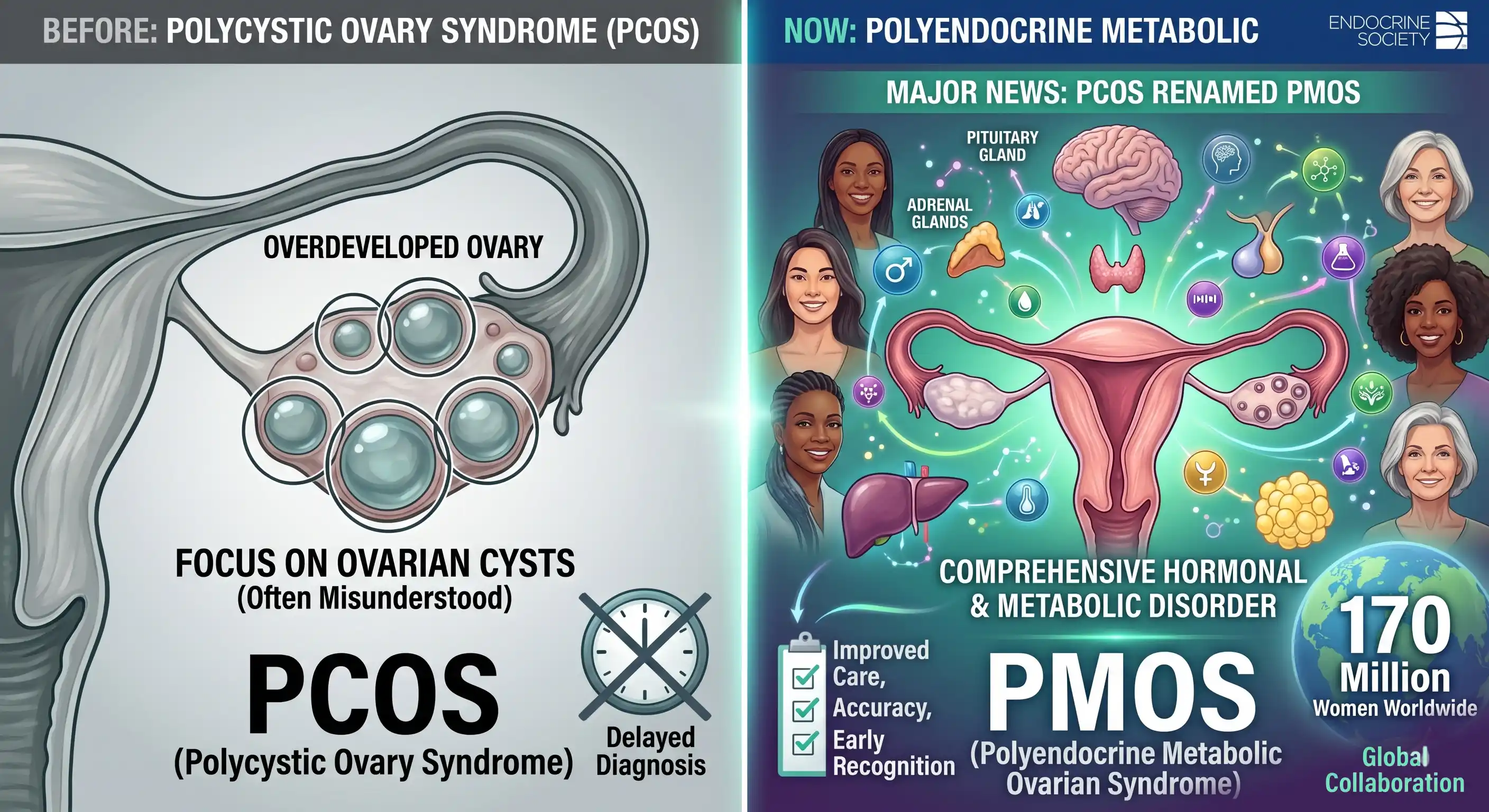
A condition affecting 1 in 8 women — more than 170 million people worldwide — has been officially renamed. According to the Endocrine Society’s press release, Polycystic Ovary Syndrome (PCOS) is now called Polyendocrine Metabolic Ovarian Syndrome (PMOS). The change was published in The Lancet on May 12, 2026, and led by 56 patient and professional organisations. For millions of women who spent years being misdiagnosed, dismissed or confused by a name that pointed to cysts that were never really there — this matters deeply.
What Changed — and Why It Took So Long
Tap each word below to understand what the new name actually means.
PMOS Is Not Just an Ovarian Condition
Tap a body region to see which systems PMOS affects beyond the reproductive organs.
to explore how PMOS affects each body system — far beyond what its old name suggested.
PMOS is associated with higher rates of anxiety, depression and negative body image. The WHO notes that women with PCOS experience a range of mental health problems — including anxiety, depression and eating disorders — at significantly higher rates than those without the condition. Mental health screening is considered as important as metabolic monitoring in comprehensive PMOS care.
Excess androgens — male hormones present in all women but elevated in PMOS — cause acne, excess facial or body hair (hirsutism) and scalp hair thinning. These are often the first visible signs, yet are frequently dismissed as cosmetic concerns rather than indicators of a systemic hormonal condition. The WHO lists excess hair and acne among the defining symptoms of the condition.
PMOS involves disruptions across multiple hormone systems — not just reproductive hormones. Insulin, LH (luteinising hormone), FSH, androgens and cortisol can all be dysregulated. The Endocrine Society notes this polyendocrine nature is central to why the old name was inadequate — it pointed only to the ovaries while the broader endocrine system was being disrupted.
PMOS raises the risk of hypertension, dyslipidaemia (abnormal cholesterol) and cardiovascular disease. The WHO identifies cardiovascular disease as a key long-term risk for women with PCOS. Research covered in KarmActive’s hypertension coverage notes that metabolic conditions compound cardiovascular risk — particularly in women who go undiagnosed for years.
Insulin resistance is a prominent feature of PMOS, with research estimating its prevalence between 35% and 80% depending on population and obesity status. It drives weight gain, difficulty losing weight, type 2 diabetes risk and non-alcoholic fatty liver disease. The CDC identifies PCOS as a diabetes risk factor. The new name’s “Metabolic” component directly acknowledges this dimension.
Not all cases of PMOS involve ovarian cysts; the classic ultrasound finding reflects arrested follicles rather than true pathological cysts. Arrested follicles are eggs that failed to fully mature due to hormonal disruption — they are not the same as pathological cysts, which can rupture, bleed and require surgery. This causes irregular or absent periods and can affect fertility. The Monash PCOS Guidelines outline current evidence-based reproductive care, including guidance for those trying to conceive.

The diagnostic criteria for PMOS have not changed. Women already diagnosed with PCOS do not need to repeat any tests. The condition is still identified using the same clinical markers: irregular periods, elevated androgen levels and the presence of multiple arrested follicles on ultrasound. What has changed is how the condition is framed — and that framing matters for how seriously it is taken by both patients and healthcare providers.
Researchers behind the renaming also found no increase in true pathological ovarian cysts in PMOS patients compared to the general population. True pathological cysts — which can rupture, bleed and require surgery — are a distinct condition. The term “polycystic” was always a misnomer, rooted in early surgical observations from 1935. Correcting it, nearly a century later, is the result of painstaking international consensus-building, not a quick editorial decision.
A Timeline of the Renaming Journey
Tap each milestone to expand the story.
From the People Who Made It Happen
What we now know is that there is actually no increase in abnormal cysts on the ovary, and the diverse features of the condition were often unappreciated.
This is about accountability and progress. It is about my daughters, their daughters, and the countless women yet to be born. We deserve clarity, understanding, and equitable healthcare from the very beginning.
It is fantastic that the new name now leads with hormones and recognizes the metabolic dimension of the condition. This shift will reframe the conversation and demand that it is taken as seriously as the long-term, complex health condition it is.
It was essential that the new name was scientifically correct but also considered across diverse cultural contexts to avoid certain reproductive terms that could heighten stigma and be harmful for women in some countries.
India’s High and Variable Burden — And Why Clearer Terminology Matters Here
India has a high and variable burden of PCOS/PMOS, with studies reporting prevalence from 3.7% to 22.5% depending on population and diagnostic criteria, according to the Indian Journal of Medical Research. The Indian Council of Medical Research (ICMR) has identified wide regional variation and warned of increasing metabolic complications among Indian women with the condition.
Research from the ICMR-supported multicentre study notes the condition runs parallel to a rise in non-communicable diseases in India, particularly type 2 diabetes. Indian women with PMOS face higher rates of obesity, dyslipidaemia and metabolic syndrome than global averages suggest. Mental health burdens like diabetes burnout compound these challenges, as covered by KarmActive. In many communities, open conversations around menstrual and reproductive health remain limited — making clearer, stigma-free terminology particularly relevant.
Treatment Hasn’t Changed. The Approach Has.
Management strategies remain the same — but the new name is expected to ensure all dimensions are treated, not just fertility.
The renaming of PCOS to Polyendocrine Metabolic Ovarian Syndrome (PMOS) was covered across this piece — including the 14-year global process that produced it, the six body systems affected, the latest statistics on the diagnosis gap, India’s specific prevalence data, and the voices of the researchers and patients who drove the change. The condition’s diagnostic criteria, treatment strategies and core clinical features were also reviewed. A three-year transition period is now underway, with full adoption expected in the 2028 International Guideline update.
For more on science and health stories that matter, explore KarmActive’s Science & Health coverage and the latest at KarmActive.com.