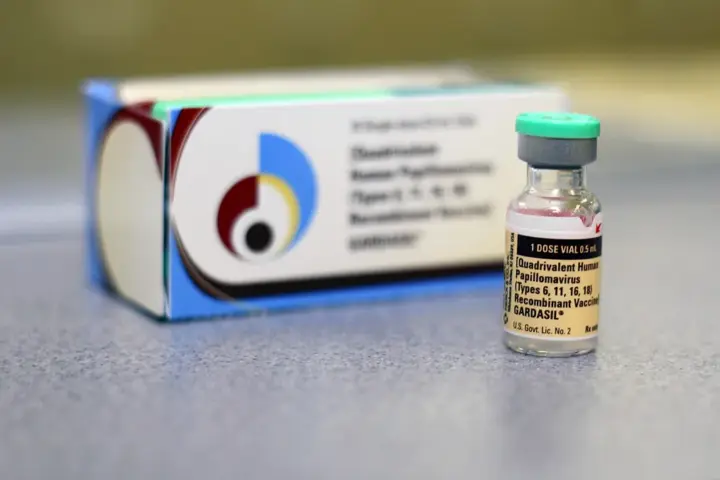
Photo Source: Sandip Dey, Wikimedia Commons, CC BY-SA 4.0 | Salt evaporation pans at Marakkanam, Tamil Nadu — where seawater is processed into salt, reflecting a broader pattern of salinity now measurable in drinking water sources across coastlines worldwide.
Health & EnvironmentSaltwater in Your Glass: How Rising Seas Are Quietly Raising Blood Pressure Worldwide
A global meta-analysis of 74,063 people links drinking water salinity to a 26% higher risk of hypertension — and the effects are most pronounced in coastal populations, many of whom rely on groundwater as their primary source.
Most people tracking their blood pressure watch what they eat. But for the more than three billion people living in coastal or near-coastal regions, a portion of daily sodium intake may be arriving through an unexpected route — the water they drink and cook with, in areas where groundwater is vulnerable to salinity intrusion.
A systematic review and meta-analysis published in BMJ Global Health on December 10, 2025, examined data from 27 population-based studies covering 74,063 participants across the United States, Australia, Israel, Bangladesh, Vietnam, Kenya, and several European countries. The study — with Dr. Rajiv Chowdhury, chair of the Department of Global Health at Florida International University’s Robert Stempel College of Public Health, as senior author — asked whether saltier drinking water increases blood pressure and hypertension risk.
The answer, consistently, was yes. People consuming higher-salinity water showed higher average blood pressure readings and a statistically significant increase in hypertension risk — with the strongest and most consistent associations observed among coastal populations where seawater intrudes into freshwater aquifers.
This matters beyond individual diet choices. Hypertension affects over one billion people globally and remains a leading cause of heart disease and stroke. Prevention efforts have historically focused on lifestyle — diet, exercise, smoking. Environmental exposure to sodium from drinking water has received comparatively little attention. This research adds a measurable dimension to that gap.
What the Numbers Show
Study findings from 74,063 participants across 27 observational studies — drag the slider to explore relative exposure levels
Systolic Blood Pressure
Diastolic Blood Pressure
developing hypertension
The mechanism is direct: higher salinity in water means more dissolved sodium. Unlike food, salty water often cannot be detected by taste at lower concentrations — meaning people in affected areas may be accumulating additional sodium intake without realising it, on top of what they consume through meals. The researchers found that the study’s 26% higher hypertension risk was statistically significant (pooled OR 1.26; 95% CI 1.07–1.48).
For most people, food is the primary sodium source. But when groundwater salinity is elevated, drinking and cooking with that water can increase total sodium intake. The World Health Organization recommends a maximum of 5g of salt per day — a limit already exceeded by much of the global population through diet alone.
A Risk on Par with Being Sedentary
How does salty water compare in magnitude to other known hypertension risk factors?
Over 1 billion people globally live with hypertension. World Heart Federation data shows cardiovascular disease causes more deaths worldwide than any other condition. Environmental sodium exposure adds a layer that current clinical guidelines do not formally address.
The World Health Organization currently has no formal health-based sodium limit for drinking water. The WHO’s guideline sets an “aesthetic objective” of 200 mg/L based on taste, not on health evidence. The 2025 meta-analysis is part of growing scientific calls to establish clinical thresholds for sodium in drinking water.
Over three billion people live in coastal or near-coastal regions globally. Many are in low- and middle-income countries where groundwater is the primary drinking source — though not all of these populations are exposed to saline water. Areas where groundwater salinity is elevated are the specific concern, including parts of India, Bangladesh, Vietnam, and Kenya.
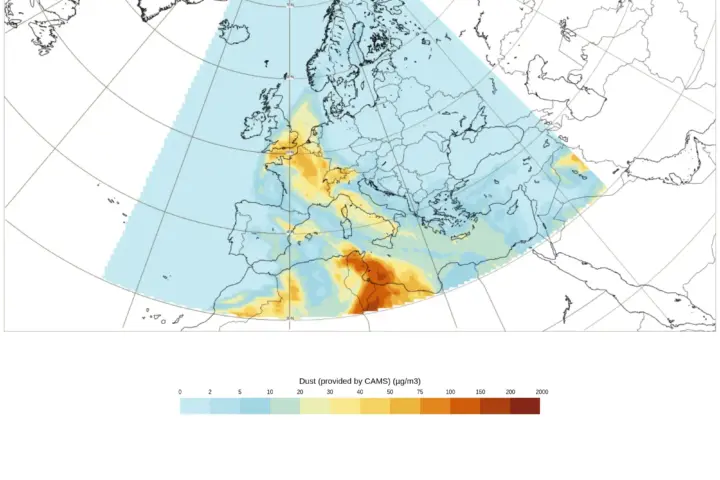
What Is Pushing Saltwater Inland
Saltwater intrusion into freshwater aquifers is driven by multiple overlapping forces — not rising seas alone
As global sea levels rise, seawater pushes further inland, contaminating freshwater aquifers in low-lying coastal zones. IPCC Sixth Assessment Report projections indicate this intrusion will intensify with continued warming. Coastal Bangladesh, the Mekong Delta, and the Indian Sundarbans are among the most documented affected areas. Ocean circulation changes may further reshape salinity patterns across these regions.
In coastal cities, heavy extraction of freshwater for urban and industrial use creates pressure differentials that draw seawater into the aquifer from the ocean side. USGS documentation on saltwater intrusion covers this pattern across multiple US coastal regions. Groundwater extraction globally has been shown to have measurable effects on subsurface water balance.
In Vietnam’s Mekong Delta, conversion of rice paddies to saltwater shrimp ponds has been documented by environmental agencies as a major driver of soil and groundwater salinisation, affecting drinking wells in nearby communities. In Bangladesh, reduced freshwater flow through transboundary rivers — influenced in part by upstream infrastructure — has allowed the Bay of Bengal to push inland, with saline water in some studies reported to extend over 100 km inland during dry periods, though the extent varies by season and location. For broader context on regional drying trends that compound these pressures, see earlier KarmActive coverage.
Where the Risk Is Most Documented
Select a region to see study-specific context from the meta-analysis and supporting research
“These are modest increases at the individual level, but when large populations are exposed, even small shifts in blood pressure can have significant public health effects. To put it in perspective, the risk level observed in this study for water salinity is like other established cardiovascular risk factors, such as low physical activity, which increases hypertension risk by approximately 15 to 25%.”
— Dr. Rajiv Chowdhury, Senior Author & Chair of Global Health, Florida International University (FIU News Release, January 26, 2026)
The research also points to specific populations facing compounded risk. A case-control study by Khan et al., published in PLOS ONE in 2014 and conducted in Dacope, Bangladesh, among 202 pregnant women and 1,006 matched controls, found that adjusted risks for pre-eclampsia and gestational hypertension increased in a dose-response pattern with rising sodium concentrations in drinking water, with adjusted odds ratios reaching as high as 5.48 at the highest salinity levels tested (above 900 mg/L). These figures represent upper-range associations from a single-area case-control study and are not a universal estimate across all coastal populations.
In Kenya, a separate cross-sectional study by Rosinger et al., published in Science of the Total Environment in 2021, examined Daasanach pastoralist communities near Lake Turkana in northern Kenya. That study — which is independent of the 2025 meta-analysis — found that higher drinking water salinity was associated with higher odds of hypertension and with hyperdilute urine (urine specific gravity below 1.003 g/mL, a marker of altered kidney function), with each additional 100 mg/L of salinity linked to 45% higher odds of hypertension in adjusted models. The prevalence of hyperdilute urine among adults in the study cohort was 30.7%.
On the question of which populations are most affected within the meta-analysis, some subgroup analyses suggest stronger associations in certain Asian populations — including those in coastal delta regions like the Mekong and Ganges-Brahmaputra — though this is not a universally confirmed finding across all studies in the pool.
India’s coastal groundwater situation is directly relevant. The Central Ground Water Board documents salinity intrusion across coastal districts in Gujarat, Tamil Nadu, Odisha, West Bengal, and Andhra Pradesh. With millions dependent on shallow wells in these areas, water quality intersects with the cardiovascular health burden already relevant to India’s Jal Shakti policy agenda. Environmental exposure risks like air pollution are increasingly understood to compound the same cardiovascular vulnerabilities in the same populations.
The researchers also found insufficient evidence to draw conclusions about other cardiovascular outcomes, such as heart attack or stroke. Long-term data linking drinking water salinity to these endpoints remains a gap they describe as a priority for future research, alongside establishing dose-response relationships between specific salinity concentrations and blood pressure outcomes. The UN Water fact sheet on water and climate change places saltwater intrusion within the broader climate-health nexus, with sea-level projections from the IPCC AR6 indicating that the frequency and geographic reach of intrusion events is expected to grow.
What People in Coastal Areas Can Do
Sodium management, the researchers say, must account for water quality alongside diet
If you live within 50 km of a coast and rely on a well or local groundwater, check for Electrical Conductivity (EC) or Total Dissolved Solids (TDS). Health effects may occur below the 200 mg/L taste threshold in some cases. India’s Water Index from NITI Aayog provides state-level groundwater quality data.
Groundwater salinity is not constant. It tends to rise during dry months when river freshwater flow decreases and seawater pushes further inland. People with existing hypertension should be more attentive to water quality and sodium intake during these periods.
In parts of coastal Bangladesh, some intervention studies have associated a switch to collected rainwater with lower blood pressure compared to groundwater use. In areas without piped supply, UNESCO water security guidance includes decentralised options such as rainwater collection as part of safe water access strategies.
Standard low-sodium dietary advice remains the foundation. But if your water source is saline, your total sodium intake may be higher than food labels suggest. A doctor can factor water-borne sodium into blood pressure management, measured against the WHO’s 5g daily limit.
The systematic review and meta-analysis examined the relationship between drinking water salinity and blood pressure across 27 population-based studies involving 74,063 participants from seven countries. The pooled findings associated higher sodium concentrations in water with an average increase in both systolic and diastolic blood pressure, and a 26% higher risk of hypertension overall (pooled OR 1.26; 95% CI 1.07–1.48).
The review identified that these effects were most consistent among coastal populations and were strongest in studies published since 2010. The discussion included the role of sea-level rise and saltwater intrusion as contributing environmental factors, alongside anthropogenic drivers such as aquifer over-extraction and agricultural land-use changes. Noted research limitations included a lack of long-term data on cardiovascular events and the absence of existing WHO health-based standards for sodium in drinking water.
For further context on environmental health risks and water quality, see KarmActive’s coverage of emerging water treatment research, waterborne contamination risks, and the broader climate indicators shaping environmental health.